During the past decade or two, the field of biomarkers (short for biological markers) has witnessed immense development.
The complexity of the field mirrors its multi-faceted applications, and it is easy to get confused with the different terms used in different contexts.
This article will help make things clearer by explaining “What is a biomarker?”, the different types of biomarkers, the key characteristics of biomarkers, and their uses in disease research.
What is a Biomarker?
What is a Biomarker?
A biomarker is a molecular, cellular, or biochemical change that can be accurately and repeatably measured and can be used to identify and monitor physiological and pathogenic processes or responses to pharmacological interventions. [1]
Put this article into practice
Choose a free resource to help you move forward
DOWNLOAD
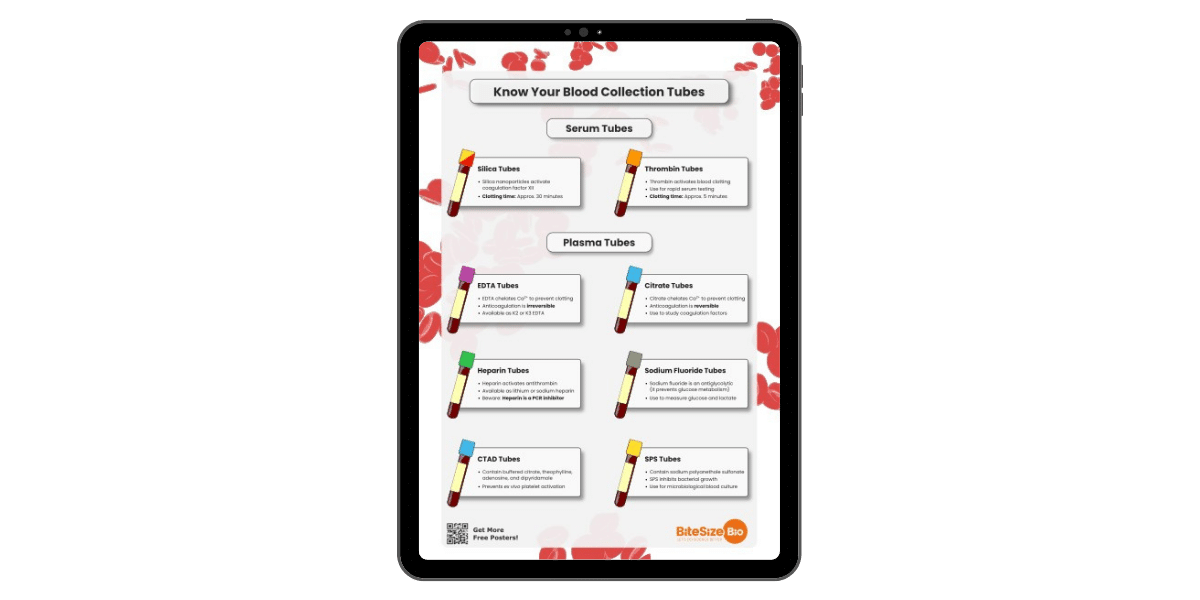
Blood Collection Tube Chart
CHEAT SHEET
Nuclear Extraction Protocol
The key message here is that biomarkers help not only in disease diagnosis (diagnostic biomarkers) but also in identifying potential treatments and tracking disease progression, regression, and outcome after an intervention.
Biomarkers include biomolecules like carbohydrates, proteins, lipids to genes, DNA, RNA, platelets, enzymes, hormones, etc. Anything that helps in the identification of a disease can serve as a biomarker, be it a metabolite, a change in biological structure or biological processes, or a characteristic feature. Biomarkers can be classified in many ways.
Biomarker detection can use a range of methods, from blood tests to magnetic resonance imaging (MRI), which can affect their usability.
Research Application of Biomarkers: Drug Discovery and Development
Drug discovery and development is a tricky business. Failure rates of new drugs (meaning they fail at some point during development and clinical testing) are as high as 90% and can reach even higher for certain conditions like Alzheimer’s disease.
Identifying reliable biomarkers can aid drug discovery and potentially increase success rates. Let’s take a deeper look at why biomarkers are important in drug discovery.
Biomarkers play a key role in the initial phases of drug discovery and development, as they can help identify potential therapeutic targets by identifying molecular pathways of disease. In addition, biomarkers can aid our understanding of the mechanisms of candidate therapeutics, which can further help assess the validity of potential therapeutics.
Biomarkers are also vital in later stages of drug development and are used in clinical research and clinical trials to assess response to treatments.
Types of Biomarkers
Types of Biomarkers
There are numerous ways to classify biomarkers. Read on to discover the various ways biomarkers are classified and how this relates to disease identification, progression, and clinical outcomes.
One note of caution is that biomarkers can fall into multiple types. For example, BRCA1 expression is both a predictive biomarker and a prognostic biomarker for the response to chemotherapy in sporadic epithelial ovarian cancer. [2]
Type 0, Type1 and Type 2 Biomarkers
Type 0, Type1 and Type 2 Biomarkers
According to Genetics and Molecular Biology methods, biomarkers can be classified as follows. [3]
Type 0 Biomarkers
Type 0 Biomarkers
Also known as natural history biomarkers. These biomarkers help measure the natural history of a disease and correlate over time with known clinical indicators.
An example of a type 0 biomarker is the measurement of serum creatinine to measure kidney function or monitor injury to kidneys. [4]
Type 1 Biomarkers
Type 1 Biomarkers
These are drug activity biomarkers, and they indicate the effect of drug intervention. They may be further divided into: [5]
- Efficacy biomarkers – indicating the therapeutic effects of a drug;
- Mechanism biomarkers – giving information about the mechanism of action of a drug;
- Toxicity biomarkers – indicating the toxicological effects of a drug.
Examples of type 1 biomarkers include blood glucose levels (efficacy biomarker) to monitor the effects of insulin treatment [4] and cytokines (mechanism biomarker) in autoimmune diseases such as rheumatoid arthritis. [6]
Type 2 Biomarkers
Type 2 Biomarkers
These are surrogate markers (also known as surrogate endpoints) that serve as a substitute for a clinical outcome of a disease and also help predict the effect of a therapeutic intervention. Such markers may correlate with clinical endpoints but may not have a guaranteed relationship.
Cholesterol in heart disease is one example of a Type 2 biomarker—where elevated levels are correlated with increased risk of heart disease, but the relationship is not always present, as there are cases of heart disease with low cholesterol levels, and some patients do not develop heart disease despite high levels of cholesterol.
Prognostic, Predictive, Pharmacodynamic and Surrogate End-point Biomarkers
Prognostic, Predictive, Pharmacodynamic and Surrogate End-point Biomarkers
- Prognostic.
- Predictive.
- Pharmacodynamic.
- Surrogate end-point.
Prognostic Biomarkers
Prognostic Biomarkers
Prognostic (Greek) means “fore-knowing or foreseeing.” Prognostic biomarkers are the ones that suggest the likely outcome of a disease in an untreated individual.
An example of a prognostic biomarker is the mutation status of PIK3CA in HER-2 positive metastatic breast cancer, where individuals with mutated PIK3CA have been found to have lower rates of disease-free survival. [7]
Predictive Biomarkers
Predictive Biomarkers
Predictive biomarkers are used to identify those patients who are likely to have a positive clinical outcome in response to a given treatment. Thus, with the help of predictive biomarkers, it is possible to give a particular therapy to the patients for which it is most likely to be effective.
Erlotinib maintenance treatment is a therapeutic intervention used to treat advanced non–small-cell lung cancer. For patients with an EGFR mutation in the tumor, progression-free survival is significantly lower following erlotinib treatment than for those without an EGFR mutation receiving the same treatment. This makes EGFR mutation status a predictive biomarker for response to erlotinib treatment.
Pharmacodynamic Biomarkers
Pharmacodynamic Biomarkers
These biomarkers help in determining the pharmacological effects of a drug and can inform if the treatment is working as expected.
PI3K inhibitors are used to treat a variety of cancers. The PI3K signaling pathway includes multiple downstream targets, including AKT. On activation of the PI3K pathway, AKT becomes phosphorylated, and therefore phosphorylated AKT (pAKT) can act as a pharmacodynamic biomarker to confirm that Pi3K inhibitor treatment is indeed inhibiting the PI3K pathway. [8] If pAKT levels drop, the inhibitor is working.
Surrogate Biomarkers
Surrogate Biomarkers
Surrogate biomarkers are identical in all but name to type 2 biomarkers, so see the section above for more detail. Another example of a surrogate biomarker is blood pressure for cardiac disease.
To be useful, surrogate markers should be an effective substitute for the clinical outcome, and effects on the substitute should predict clinical outcomes.
However, there is a possibility, because the biomarker is just a surrogate, that the effect of pharmacological therapeutics on the surrogate may not affect the outcome, limiting its usefulness. [9]
Biomarkers of Exposure and Disease
Biomarkers of Exposure and Disease
The final way to classify biomarkers is by dividing them into two broad types: [10]
Biomarkers of Exposure
These can also be called antecedent biomarkers and are used in risk prediction.
Biomarkers of Disease
Important Characteristics of a Biomarker
Important Characteristics of a Biomarker
According to the US Food and Drug Administration (FDA), [3,5] an ideal biomarker should be:
- specific for a particular disease and able to differentiate between different physiological states;
- safe and easy to measure;
- rapid to enable faster diagnosis;
- cheap;
- able to give accurate results;
- and consistent between different ethnic groups and genders.
Different diseases have different biomarkers associated with them that are specific to that particular disease.
Examples of Biomarkers
Some examples of the different types of biomarkers discussed are:
- Blood glucose levels: A type 1 biomarker (efficacy biomarker) for monitoring the effects of insulin treatment in diabetes.
- PIK3CA mutation status in HER-2 positive breast cancer: A prognostic biomarker indicating disease outcome in untreated individuals.
- EGFR mutation status in non-small-cell lung cancer (NSCLC): A predictive biomarker for response to erlotinib treatment, guiding personalized therapy selection.
- Phosphorylated AKT (pAKT) levels: A pharmacodynamic biomarker confirming the inhibition of the PI3K pathway by PI3K inhibitors in cancer treatment.
- Blood pressure: A surrogate biomarker for cardiac disease, aiming to predict clinical outcomes based on its measurement.
These examples highlight the diverse classifications and applications of biomarkers in healthcare.
FAQs
Q. How do researchers ensure the specificity and accuracy of biomarkers across different ethnic groups and genders, as suggested by the FDA’s criteria for an ideal biomarker?
A. Ensuring the specificity and accuracy of biomarkers across diverse ethnic groups and genders requires rigorous validation studies involving representative populations. Researchers employ robust statistical methods to analyze data and adjust for demographic variables, ensuring the biomarker’s reliability and applicability across different groups.
Q. What challenges arise when biomarkers fall into multiple classification types, such as BRCA1 expression serving as both a predictive and prognostic biomarker for chemotherapy response in ovarian cancer?
A. Biomarkers that fall into multiple classification types pose challenges in interpretation and clinical application. Researchers must carefully consider the context and implications of biomarker measurements, understanding how they may impact treatment decisions and patient outcomes based on their dual roles in predicting disease progression and treatment response.
Q. Can surrogate biomarkers reliably predict clinical outcomes, considering the limitations posed by their potential lack of correlation with the actual disease status?
A. Surrogate biomarkers serve as substitutes for clinical endpoints, aiming to predict treatment effects or disease outcomes. However, their reliability depends on the strength of their correlation with clinical endpoints. Researchers conduct thorough validation studies to assess the surrogate biomarker’s predictive value and its ability to accurately reflect treatment efficacy or disease progression.
Biomarkers in Biological Research Summarized
Biomarkers in Biological Research Summarized
Hopefully, that answered the question “What is a biomarker?”, provided details of the various types of biomarkers along with useful examples, including several cancer biomarkers, and highlighted their importance in drug discovery and development.
Do you use biomarkers in your research? Let us know in the comments below!
Originally published July 2016. Revised and updated March 2024.
References
References
- Naylor S. (2003) Biomarkers: current perspectives and future prospects. Expert Rev Mol Diagn 3:525–29
- Carser JE, Quinn JE, Michie CO, O’Brien EJ, McCluggage WG, Maxwell P, Lamers E, Lioe TF, Williams AR, Kennedy RD, Gourley C, Harkin DP. (2011) BRCA1 is both a prognostic and predictive biomarker of response to chemotherapy in sporadic epithelial ovarian cancer. Gynecol Oncol 123(3):492–8
- Sahu P, Pinkalwar N, Dubey RD, Paroha S, Chatterjee S, Chatterjee T. (2011) Biomarkers: an emerging tool for diagnosis of a disease and drug development. Asian J Res Pharm Sci 1: 9–16
- Kaplan JM, Wong HR. (2011) Biomarker discovery and development in pediatric critical care medicine. Pediatr Crit Care Med 12(2):165–173
- Jain KK. The Handbook of Biomarkers, 2nd Ed, New York, Springer, 2017
- Robinson WH, Lindstrom TM, Cheung RK, Sokolove J. (2013) Mechanistic biomarkers for clinical decision making in rheumatic diseases. Nat Rev Rheumatol 9(5):267–276
- Seo Y, Park YH, Ahn JS, et al. (2018) PIK3CA mutations and neoadjuvant therapy outcome in patients with human epidermal growth factor receptor 2-positive breast cancer: A sequential analysis. J Breast Cancer 21(4):382–90
- Yang J, Nie J, Ma X, et al. (2019) Targeting PI3K in cancer: mechanisms and advances in clinical trials. Mol Cancer 18:26
- Fleming TR, DeMets DL. (1996) Surrogate end points in clinical trials: are we being misled? Ann Intern Med 125(7):605–13
- Mayeux R. (2004) Biomarkers: Potential uses and limitations. J Am Soc Exp Neuro Therap 1:182–88
You made it to the end—nice work! If you’re the kind of scientist who likes figuring things out without wasting half a day on trial and error, you’ll love our newsletter. Get 3 quick reads a week, packed with hard-won lab wisdom. Join FREE here.
Put this article into practice
Choose a free resource to help you move forward
DOWNLOAD
Blood Collection Tube Chart
eBook
Free Guide to PCR