Biosafety is one of those things many scientists don’t take seriously. I would guess, that like politics, there are 40% who believe biosafety is ‘over-emphasized’ and 40% who swear by biosafety. 20% are undecided.
Needless to say, I’m on the side of biosafety.
And here’s why:
“CDC announced today that approximately 75 Atlanta-based staff are being monitored or provided antibiotics because they may have been unintentionally exposed to live Bacillus anthracis (anthrax) after established safety practices were not followed.” (Emphasis is mine)
Put this article into practice
Choose a free resource to help you move forward
DOWNLOAD
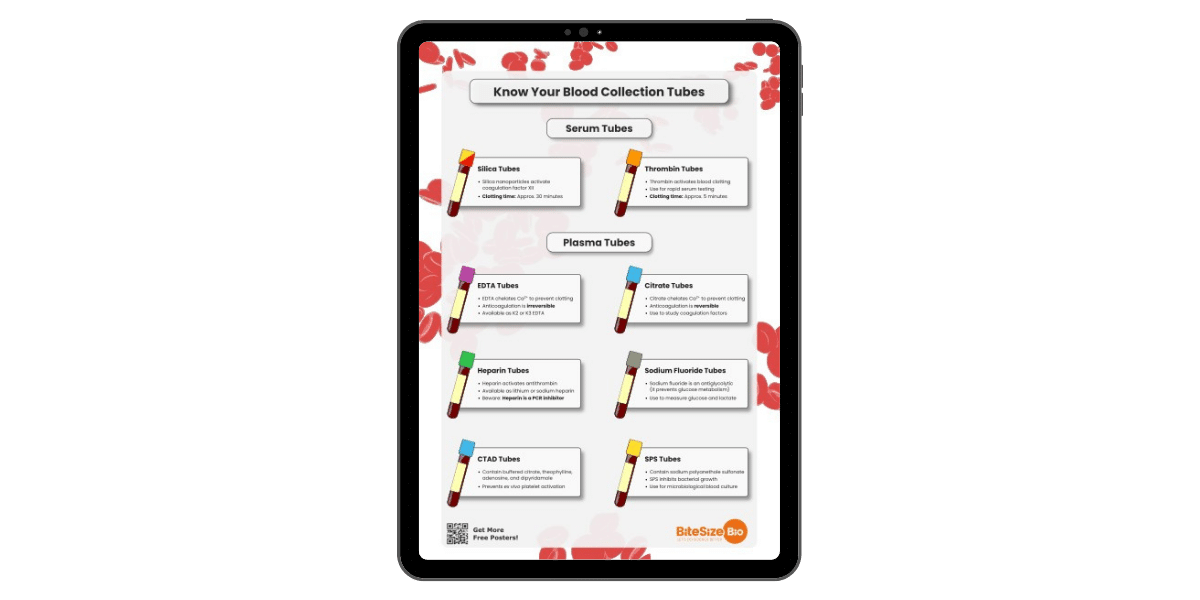
Blood Collection Tube Chart
CHECKLIST
Manuscript Summary Template and Checklist
The complete announcement can be found on the CDC website.
Yes, it can happen anywhere, including a ‘Premier’ national lab.
This is a good reminder that procedures can easily break down, or be circumvented through ignorance or malice or just someone having a bad day.
Why biosafety is important
Biosafety means putting the safety of everyone connected to your lab first – respecting his or her right to work in a safe environment.
Always.
Biosafety is also peace of mind for the lab director and the Institution. You can bet the CDC is sweating bullets on this one – they are ripe for all kinds of legal action and the director has already been ‘re-assigned’.
How to institute good biosafety practices
- Communicate. Make sure you understand and communicate the risks of each process and sample to your flow cytometrist.
- Commit. Good biosafety practices require commitment from the flow cytometrist and the administration to set rational rules and enforce them as needed. It also requires periodic review to keep protocols up to date and regular checks to ensure the rules aren’t being circumvented.
- Get to know your IBO. Each institute has its own name for the position of establishing and enforcing biosafety rules. I’ll use the term Institute Biosafety Officer (IBO) to refer to that person. With respect and common goals, it’s usually easy to have a very positive relationship with an IBO and mutually benefit from the relationship.
- Don’t be afraid to educate the IBO on the process of flow cytometry – that will help them to help you navigate the myriad of rules, regulations, assessments and classifications that make up a biosafety assessment.
Instituting biosafety protocols for flow cytometry
Follow these suggestions for good biosafety practices:
- Flow cytometrists should become acquainted with their institution’s IBO (and if there is no IBO, consider instituting some protective measures).
- Educate the IBO about the flow cytometry process, and let the IBO teach you about risk assessment, and institutional and governmental requirements.
- Consider all possible angles, brainstorm, and seek outside opinions to formulate a robust policy. If possible, conduct walk-throughs and ‘test’ scenarios and REVIEW them over time to be sure they work. And lastly, ENFORCE them.
- Also keep in mind that flow cytometric analysis has very different requirements and assessment than cell sorting.
Analytical analysis
In tracing the fluidics pathway, it is important to remember that with analytical flow cytometers, the fluidics path is closed, so the cells pass from the tube past the intercept point and into the waste all in a sealed path.
Thus, biosafety concerns should focus on sample preparation and presentation to the instrument/facility. Important considerations include:
- How are the prepared cells transported from the processing site to the flow cytometer?
- How will the samples will be fixed before running ?
- If it is not possible to fix the samples, what extra precautions will be taken when unfixed, higher risk samples are presented to the facility.
Cell sorting
In cell sorting, especially electrostatic cell sorting, the cell stream is broken into droplets. Most systems can generate 90,000 or more droplets per second. Any one of these aerosolized droplets could contain a specific cell that might be infectious.
This fact demands that a complete risk assessment be performed on the processes and procedures that are put in place for sorting those cells deemed at higher risk (BSL2 and higher).
Know what you are working with. In the case of cell sorting, knowledge of the cells to be sorted is absolutely necessary. The protection of the sort operator is critical, and knowledge will allow for the proper assessment of bio-containment and safety. It is recommended that there is a document trail for the operator to review before the cells are sorted.
Address inherent dangers of generating aerosols by using proper protocols, engineering controls and personal protective equipment.
Don’t be the shining example of the CDC.
References
- Holmes, KL, et al., (2014) International society for the advancement of cytometry cell sorter biosafety standards. Cytometry A 85A;434-453.
- Schmid, I. et al., (2007) International society for analytical cytology biosafety standard for sorting of unfixed cells. Cytometry A 71A:414-437.
- Schmid, I, et al., (1997) Biosafety guidelines for sorting of unfixed cells. Cytometry 28:99-117.
You made it to the end—nice work! If you’re the kind of scientist who likes figuring things out without wasting half a day on trial and error, you’ll love our newsletter. Get 3 quick reads a week, packed with hard-won lab wisdom. Join FREE here.
Put this article into practice
Choose a free resource to help you move forward
DOWNLOAD
Blood Collection Tube Chart
POSTER
Cell Culture Posters