When choosing a model system for studying anti-angiogenic therapy for cancer treatment, one instantly thinks of using an in vitro assay (cell culture) or a more complex in vivo model system, such as mice or rats. What if there were another well-established method to study angiogenesis that combines the simplicity of cell culture when it comes to handling with the sophistication of in vivo models?
Chick embryo chorioallantoic membrane (CAM) is a widely used tool to assess both angiogenesis and anti-angiogenic activities of compounds. [1,2] However, it seems that this method is not as well known to budding researchers. There are several reasons for and benefits of using an emerging/non-model system. In this article, we will go through the basics and methodology of the CAM assay and its use in studying angiogenesis and anti-angiogenic drugs.
Angiogenesis and Cancer Progression
Angiogenesis is the growth of new blood vessels from pre-existing vasculature. Blood capillaries are required for the exchange of nutrients and metabolites in all tissues. [3] However, the formation of new blood vessels is also required for and triggered by the nutrient and oxygen requirements of tumor tissues. [4] Thus, angiogenesis is necessary for tumor growth and metastasis (spread of cancer cells). For this reason, inhibiting angiogenesis using drugs or metabolites has been considered a possible way to control cancer progression. In fact, several anti-angiogenic drugs are approved for use in cancer therapy.
Commonly Used Models for Studying Angiogenesis
Models to study angiogenesis have been developed at various levels—organ system, tissue, cellular, and molecular. [5] In vitro models capable of mimicking certain aspects of cellular and biochemical events of angiogenesis include the Matrigel® tube-forming assay, fibrin and collagen gel-cord-forming assays, the aortic ring model, and a variety of endothelial cell proliferation assays. [2]
Put this article into practice
Choose a free resource to help you move forward
POSTER
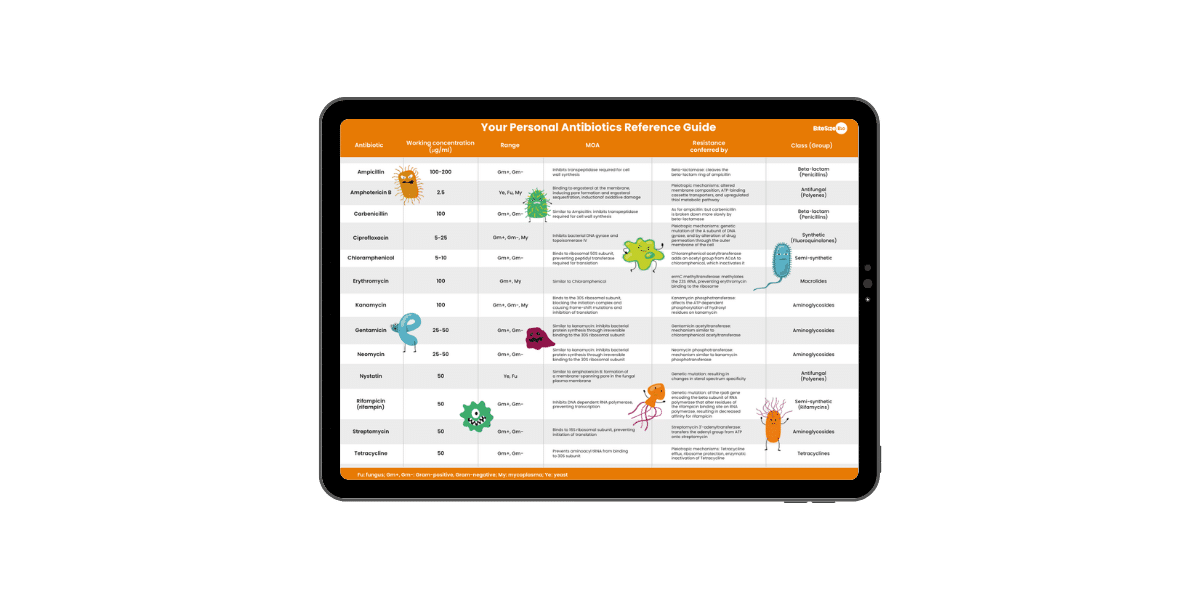
Antibiotics Reference Guide
POSTER
Cell Culture Posters
However, these models focus on single aspects of angiogenesis. Angiogenesis is a complex process that involves cell adhesion, migration, invasion, and proliferation. These steps occur in a coordinated fashion. Including all these steps in a single in vitro model is not possible. [2] This naturally makes in vivo models a preferred choice for a more comprehensive understanding.
Some in vivo models include the corneal pocket assay (in rabbit, mouse, and rat), murine Matrigel plug assay, human/mouse chimeric angiogenesis assay, primate iris neovascularization model, and the CAM assay. [2] All of these models offer the benefit of a comprehensive understanding of angiogenesis at a physiological microenvironment level. However, the CAM assay has several unique advantages, including simplicity; ease of handling; quick, reliable results; the possibility of a larger sample size; and cost. Let’s take a look at the basics and methodology of the CAM assay.
CAM Assay Basics
The CAM of the chick embryo is responsible for the exchange of gases and nutrients to the growing embryo and is a site of active vascularization. It consists of two separate membranes (the chorion and allantois) that fuse on the 4th to 5th day of incubation. [2] The assay is performed using the following steps:
Step 1: Procure and Incubate Fertilized Eggs
With a quick Google search, you can easily locate a vendor that sells fertilized eggs. Once you receive the eggs, incubate them in a ventilated incubator (even a laboratory hot air oven will work just fine as long as the temperature is well controlled) at 37°C for 3 days. Make sure you rotate the eggs at least a few times every day during this period. This prevents the embryo from adhering to the inner shell membrane and ensures healthy growth (just the way a hen turns it frequently during brooding).
Step 2: Candle the Eggs
Even if you procure eggs from a vendor who assures that the eggs are fertilized, there is a chance that a few aren’t. Confirm embryonic development by candling the eggs on day 3 of incubation. Candling is simply holding the egg against a light source such as an electric bulb, which will create a shadow of the embryo on the surface of the shell. You can either buy a candler online or you can easily create one by incorporating a bulb in a cardboard box and making a hole to place the egg on. Discard the non-viable eggs, and re-incubate those that have a developing embryo.
Step 3: Prepare the Sample Discs
The next step is to prepare the compound whose anti-angiogenic properties you wish to test by loading it onto a filter paper disc, which allows it to diffuse in a localized manner. The discs can be prepared by cutting filter paper using a punching machine. Dissolve the sample in a volatile solvent, such as petroleum ether or ethanol. Add the dissolved sample to the disc using a micropipette so that the desired quantities of the sample can be achieved upon evaporating the solvent. Once the solvent evaporates, your sample discs are ready.
Step 4: Remove Albumin
On the fifth day of incubation, move the eggs to a laminar airflow cabinet. Swab the eggs with a disinfectant, and make a hole using a pointed drill or by tapping the egg with a needle of a syringe. Withdraw the albumin (around 2 mL) from the slender end of the egg using a sterile syringe. This will help to lower the embryo from the inner surface of the egg. Seal the hole aseptically with Parafilm® by heating a microspatula on a flame and using it to smoothly liquefy and seal the Parafilm on the hole.
Step 5: Make a Window and Place the Sample Disc
Place the egg horizontally, and swab the upper surface. Cut open a rectangular window on the upper surface using a handheld mini electric drill. You can try changing the tips of the drill and find the one you are most comfortable with. In my experience, a pointed tip works the best. Gently remove the shell using sterile forceps. Once you open it, you’ll have access to the CAM (vasculature).
Choose the region of the blood vessels, and using a sterile forceps carefully place the sample discs without disturbing the blood vessels. It is advisable to include two controls: one with a blank disc to assess the effect of the disc material and another without any discs to observe normal growth.
Take a photograph of the region where you have placed the disc, for future reference. It is also wise to take a photograph before placing the disc for comparison. Once the sample is placed, seal the window aseptically using Parafilm and cloth tape. You can use the hot spatula trick to ensure the window is properly sealed. Re-incubate the eggs at 37°C until day 7.
Step 6: Re-open the Window and Observe
On day 7, aseptically remove the Parafilm to re-open the window. Carefully remove the sample disc using sterile forceps and photograph the region of the blood vessels. Compile the photographs from day 5 with the ones from day 7, and compare. Observe the growth of blood vessels and compare them with the controls. Assign a score to the blood vessel as follows: [1]
Observations on CAM after treatment
| Score
|
No changes observed | 0 |
Minor changes (growth) in blood vessels | 0.5 |
Substantial changes: capillary-free area below the disc, few microvessels converge, and/or the growth of blood vessels slightly reduced | 1 |
Significant changes: capillary-free area below the disc, absence of microvessels, and convergence of large vessel | 2 |
Once you have assigned a score for each egg, compute the mean score (\(X\)) for the samples. Use the mean score to determine the anti-angiogenic activity of your sample based on the following criteria: [1]
\( X < 0.5 = \) No anti-angiogenic activity
\( 0.5 \leq X \leq 1 = \)Weak anti-angiogenic activity
\( 1 < X < 1.5 = \)Good anti-angiogenic activity
\( X \geq 1.5 =\) Strong anti-angiogenic activity
Isn’t it a simple assay? Next time you decide to study angiogenesis/anti-angiogenic activity, give the CAM assay a try. Let us know in the comments what you think about it. Read our related article for more information on the dos and don’ts of the CAM assay..
References
- Seow L.J., et al. Anti-angiogenic activity of Gynura segetum leaf extracts and its fractions, J. Ethnopharmacol, 134, 2 (2011). doi:10.1016/j.jep.2010.12.007.
- Brooks P.C., et al. Use of the 10-day-old chick embryo model for studying angiogenesis., Methods Mol. Biol. (1999). doi:10.1385/1-59259-249-x:257.
- Adair, T.H., Montani, J.P. Angiogenesis. In Colloquium series on integrated systems physiology: from molecule to function, 2, 1, (2010). Morgan & Claypool Life Sciences.
- Nishida N., et al. Angiogenesis in cancer, Vasc. Health Risk Manag. 2, 3, (2006). doi:10.2147/vhrm.2006.2.3.213.
- Qutub A., et al. Multiscale models of angiogenesis, in: IEEE Eng. Med. Biol. Mag., 28, 2, (2009). doi:10.1109/MEMB.2009.931791.
You made it to the end—nice work! If you’re the kind of scientist who likes figuring things out without wasting half a day on trial and error, you’ll love our newsletter. Get 3 quick reads a week, packed with hard-won lab wisdom. Join FREE here.
Put this article into practice
Choose a free resource to help you move forward
POSTER
Cell Culture Posters
POSTER
Antibiotics Reference Guide