Whether you’re already in the field or an undergrad looking to enter the scene, here are some great places to keep up to date with the latest news and trends in stem cells.
Listen About It
For auditory learners, or people that listen to music on their way to the lab, you could switch it up by listening in to The Stem Cell Podcast instead. The podcasts include a quick science round up, discussing some of the more interesting or controversial papers and an interview with a guest scientist.
Work Your Way Through a Book
For our precious bookworms, there’s plenty of good introductory books to borrow from the library, but one that I’d recommend would be Stem Cell and Tissue Engineering by World Scientific for readers with a strong science background who are ready to dip their feet into stem cell literature.
Personally I find that I digest information better if I understand every single word on the page (when it comes to scientific literature), which means, hello smartphone. You can google any terms you don’t understand immediately instead of dragging that small nugget of confusion with you over to the next page which really makes a huge difference in your understanding at the end of the book. Let’s say you didn’t understand 2 technical terms per page and there are about 400 pages, you’d be missing out on 800 technical terms (excluding repeats of a term you didn’t know). It may be more tedious than simply reading the book, but you get more out of it if you do.
Put this article into practice
Choose a free resource to help you move forward
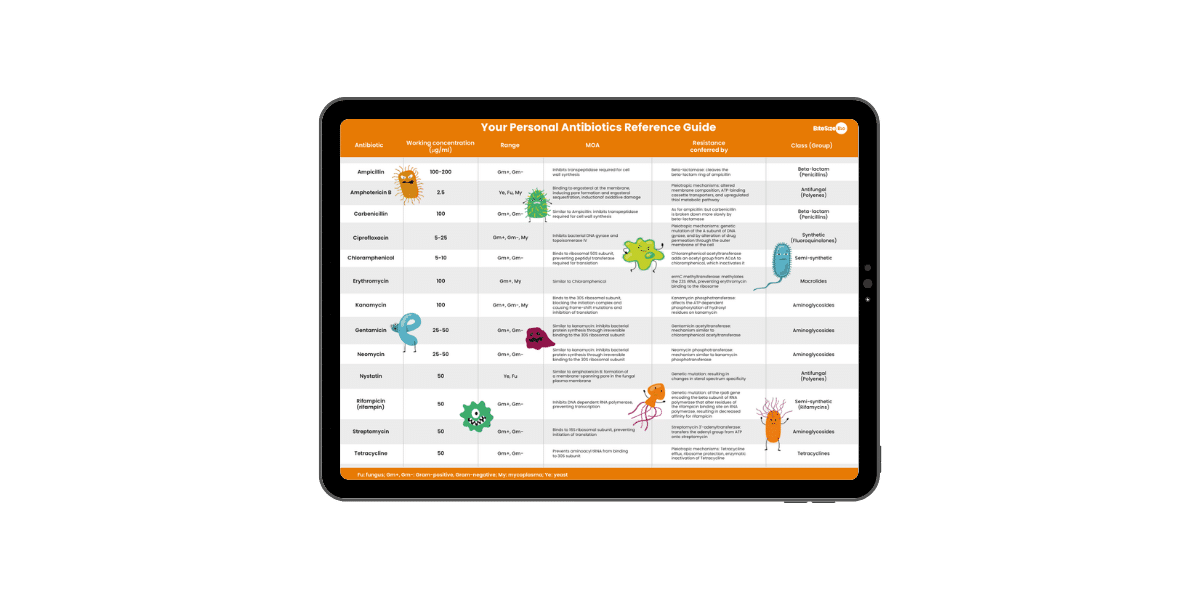
POSTER
Antibiotics Reference Guide
POSTER
Cell Culture Posters
Get Your Monthly Stem Cell Fix
For journals I would recommend heading over to Cell Stem Cell. As they describe themselves, “Cell Stem Cell is a broad-spectrum journal that covers the entire spectrum of stem cell biology. Topics covered include embryonic stem cells, pluripotency, germline stem cells, tissue-specific stem cells, stem cell differentiation, epigenetics, stem cell genomics and systems biology, genome reprogramming, cancer stem cells, stem cell niches, stem-cell-based disease models, nuclear transfer technology, bioengineering, drug discovery, in vivo imaging of stem cells, therapeutic applications, regenerative medicine, clinical and translational insights, stem cell research policies, ethical issues, and technical or resource-based innovations.” As you can tell from the introduction, they have everything you might possibly want to know about stem cells.
Ride the Information Superhighway
If you don’t have time for hitting the books or your extraordinarily large library fine has turned you into a convict, fear not. You still have the internet. There are great blogs about stem cells such as Stem Cell Assays. As taken from the blog itself, “Stem Cell Assays is a collaborative online project aimed to bring together professionals working in the field of stem cell research and cell therapy to discuss methodological issues that are holding back progress in the field.” They have a fresh take on what’s holding back research and have been mentioned in other great blogs such as The Niche written by Dr. Paul Knoepfler (@pknoepfler) who is a biomedical scientist, science writer, advocate, and cancer survivor.
And let’s not forget The Harvard Stem Cell Institute community, which features the latest in stem cell research. They also have information on their various programs which includes the prestigious International Harvard Stem Cell Institute Internship.
Getting out there
Lastly, for those who want to experience going to a stem cell conference, there are several recurring meetings and conferences. You could attend a conference held by the ISSCR (International Society for Stem Cell Research) – they have annual conferences with a large variety of topics with insightful talks from the experts in the field. Other conferences include those held by the Cold Spring Harbor Laboratory and Gordon conferences. The ISSCR has made it convenient to find out more about the various stem cell conferences by collating them into one page on their official website.
This list is not exhaustive and I’m sure there are other great resources that I have not mentioned. I hope you enjoy exploring through these resources as much as I do.
You made it to the end—nice work! If you’re the kind of scientist who likes figuring things out without wasting half a day on trial and error, you’ll love our newsletter. Get 3 quick reads a week, packed with hard-won lab wisdom. Join FREE here.
Put this article into practice
Choose a free resource to help you move forward
PROTOCOL
Chemically Competent Cells Protocol
POSTER
Antibiotics Reference Guide